The Treatments And Causes Of Over-Pronation Of The Feet
Pronation is the natural act of the body spreading the impact of walking, jogging or running throughout the foot evenly. As the foot strikes the ground, the ankle naturally rolls inward absorbing the shock of the ground and mobilizing to the terrain. Overpronation is when the ankle of the foot rolls in past its normal 15? of inward rotation. The cause of this could be many things such as foot type, biomechanics, or compensation strategies. People with flat feet often, although not always, overpronate.

Causes
Unless there is a severe, acute injury, overpronation develops as a gradual biomechanical distortion. Several factors contribute to developing overpronation, including tibialis posterior weakness, ligament weakness, excess weight, pes planus (flat foot), genu valgum (knock knees), subtalar eversion, or other biomechanical distortions in the foot or ankle. Tibialis posterior weakness is one of the primary factors leading to overpronation. Pronation primarily is controlled by the architecture of the foot and eccentric activation of the tibialis posterior. If the tibialis posterior is weak, the muscle cannot adequately slow the natural pronation cycle.
Symptoms
When standing, your heels lean inward. When standing, one or both of your knee caps turn inward. Conditions such as a flat feet or bunions may occur. You develop knee pain when you are active or involved in athletics. The knee pain slowly goes away when you rest. You abnormally wear out the soles and heels of your shoes very quickly.
Diagnosis
One of the easiest ways to determine if you overpronate is to look at the bottom of your shoes. Overpronation causes disproportionate wear on the inner side of the shoe. Another way to tell if you might overpronate is to have someone look at the back of your legs and feet, while you are standing. The Achilles tendon runs from the calf muscle to the heel bone, and is visible at the back of the ankle. Normally it runs in a straight line down to the heel. An indication of overpronation is if the tendon is angled to the outside of the foot, and the bone on the inner ankle appears to be more prominent than the outer anklebone. There might also be a bulge visible on the inside of the foot when standing normally. A third home diagnostic test is called the ?wet test?. Wet your foot and stand on a surface that will show an imprint, such as construction paper, or a sidewalk. You overpronate if the imprint shows a complete impression of your foot (as opposed to there being a space where your arch did not touch the ground).

Non Surgical Treatment
Adequate footwear can often help with conditions related to flat feet and high arches. Certified Pedorthists recommend selecting shoes featuring heel counters that make the heel of the shoe stronger to help resist or reduce excessive rearfoot motions. The heel counter is the hard piece in the back of the shoe that controls the foot?s motion from side-to-side. You can quickly test the effectiveness of a shoe?s heel counter by placing the shoe in the palm of your hand and putting your thumb in the mid-portion of the heel, trying to bend the back of the shoe. A heel counter that does not bend very much will provide superior motion control. Appropriate midsole density, the firmer the density, the more it will resist motion (important for a foot that overpronates or is pes planus), and the softer the density, the more it will shock absorb (important for a cavus foot with poor shock absorption) Wide base of support through the midfoot, to provide more support under a foot that is overpronated or the middle of the foot is collapsed inward.
Prevention
Wearing the proper footwear plays a key role as a natural way to help pronation. Pronated feet need shoes that fit well, provide stability, contain supportive cushioning, are comfortable and allow enough room for your foot to move without causing pain or discomfort. Putting special inner heel wedges, known as orthotics, into your shoes can support a flatfoot while lowering risks of developing tendinitis, according to the American Academy of Orthopaedic Surgeons. More extensive cases may require specially fitted orthopaedic shoes that support the arches.
Bunions Causes Indicators And Remedies
Overview
 Bunions are probably the most common deformity seen in the adult foot. The term ?bunion? is actually Latin for turnip. The scientific phrase used to describe a bunion is hallux valgus. Hallux is Latin for great toe, while valgus means deviation towards the outer side of the body. Bunions come in all shapes and sizes. This causes significant variation in symptoms and also in the extent of the surgery required to correct a bunion. Most patients who have symptomatic bunions complain of pain on the medial, or inner aspect of the big toe. However, bunions may also cause pain underneath the big toe, or even under the second toe.
Bunions are probably the most common deformity seen in the adult foot. The term ?bunion? is actually Latin for turnip. The scientific phrase used to describe a bunion is hallux valgus. Hallux is Latin for great toe, while valgus means deviation towards the outer side of the body. Bunions come in all shapes and sizes. This causes significant variation in symptoms and also in the extent of the surgery required to correct a bunion. Most patients who have symptomatic bunions complain of pain on the medial, or inner aspect of the big toe. However, bunions may also cause pain underneath the big toe, or even under the second toe.
Causes
There are many reasons why this deformity occurs such as hereditary factors. Footwear habits. Foot type. Biomechanical factors (pronation). Neuromuscular dysfunction. Ligament Dysfunction (laxity). The most common causative factor is inheriting a foot type from your family that is prone to bunions. Feet that are subjected to pronation also have a higher incidence of attaining HAV deformities. This is a problem that has many causes and more than one may be occurring at the same time.
Symptoms
Symptoms of a bunion include irritated skin, sensitivity to touch, and pain when walking or running. Since the bunion may grow so prominent as to affect the shape of the foot, shoes may no longer fit properly, and blisters may form at the site of friction and pressure. Bunions may grow so large that an individual must wear shoes that are a larger size than they would otherwise wear. If the bunion becomes a severe case, walking may become difficult.
Diagnosis
Although bunions are usually obvious from the pain and unusual shape of the toe, further investigation is often advisable. Your doctor will usually send you for X-rays to determine the extent of the deformity. Blood tests may be advised to see if some type of arthritis could be causing the pain. Based on this evaluation, your doctor can determine whether you need orthopaedic shoes, medication, surgery or other treatment.
Non Surgical Treatment
The treatment method your doctor chooses for you will be based on the severity of the bunion. Treatment can be simple and non-surgical or it can be complex, surgical, and costly. A bunion is permanent unless surgery is performed to remove it, but self-care can help to improve your symptoms. If you suspect that a bunion is developing, you should seek medical attention immediately. Here are the most common conservative treatment options. Changing your shoes. Adding custom orthotics to your shoes. Medication such as Tylenol for pain relief. Padding and taping to put your foot in its normal position. Applying ice or cold compresses to reduce swelling and pain. Keeping pressure off your affected toe, especially if there is swelling, redness, and pain. Before bed, separate the affected toe from the others with a foam-rubber pad and leave it there while you sleep. 
Surgical Treatment
If these methods fail, then surgery may be suggested. Basically, bunion surgery is performed to improve function or to prevent pain from occurring. When surgery is delayed in a symptomatic foot, greater amounts of arthritis can develop and the more complicated surgery can become. Surgery is performed to improve alignment and function to the big toe joint. The large bump is removed and, sometimes, a cut is made into the bone, to move it to a more normal position. Screws, pins and wires can be used beneath the skin, to improve healing and results. Healing can range from 3-12 weeks, depending on the procedure.
Prevention
Proper footwear may prevent bunions. Wear roomy shoes that have wide and deep toe boxes (the area that surrounds the toes), low or flat heels, and good arch supports. Avoid tight, narrow, or high-heeled shoes that put pressure on the big toe joint. Medicine will not prevent or cure bunions.
Tips On How To Diagnose Calcaneal Apophysitis?
Sever's disease, or calcaneal apophysitis, is a common cause of heel pain among active children between 10 to 13 years old. This spontaneous heel pain results from injury to the heel bone?s growth plate which is caused by overuse rather than specific injury or trauma. The condition is common among athletic children, particularly those active in soccer, football, and baseball. Treatment is available to reduce pain and discomfort associated with Sever's disease, but the condition usually resolves on its own once feet stop growing.
Causes
The heel bone sometimes grows faster than the leg muscles (including the calf muscles) and tendons (including the Achilles tendon) during the early puberty growth spurt. The different growth rate in these structures can cause lower leg muscles and tendons to become overstretched and tight, which makes the heel less flexible and puts excessive pressure on the heel growth plate. The Achilles tendon, the strongest tendon in the body, attaches to the heel growth plate, and repetitive stress on this structure, especially if it?s already tight, can damage the growth plate, leading to tenderness, swelling, and pain. Activities that involve running or jumping, such as soccer, gymnastics, track, and basketball, can place significant stress on a tight Achilles tendon and contribute to the onset of Sever?s disease. Ill-fitting shoes can also contribute to this health problem by failing to provide the right kind of support or by rubbing against the back of heel. The following factors may increase the likelihood of Sever?s disease in kids or young teens. Wearing footwear that is too narrow in the toe box. Leg length inequality. Obesity or carrying excess bodyweight. Excessive foot and ankle pronation.
Symptoms
Symptoms include Heel Pain. Pain at the back of the heels when walking or running. Possibly a lump at the back of the heel, although this might be minimal. Pain and tenderness at the back of the heels, especially if you press on it, or give it a squeeze from the sides. Tight calf muscles resulting in reduced ankle range of motion.
Diagnosis
A doctor can usually tell that a child has Sever's disease based on the symptoms reported. To confirm the diagnosis, the doctor will probably examine the heels and ask about the child's activity level and participation in sports. The doctor might also use the squeeze test, squeezing the back part of the heel from both sides at the same time to see if doing so causes pain. The doctor might also ask the child to stand on tiptoes to see if that position causes pain. Although imaging tests such as X-rays generally are not that helpful in diagnosing Sever's disease, some doctors order them to rule out other problems, such as fractures. Sever's disease cannot be seen on an X-ray.
Non Surgical Treatment
The following are different treatment options. Rest and modify activity. Limit running and high-impact activity to rest the heel and lessen the pain. Choose one running or jumping sport to play at a time. Substitute low-impact cross-training activities to maintain cardiovascular fitness. This can include biking, swimming, using a stair-climber or elliptical machine, rowing, or inline skating. Reduce inflammation. Ice for at least 20 minutes after activity or when pain increases. Nonsteroidal anti-inflammatory drugs (NSAIDs) may also help. Stretch the calf. Increase calf flexibility by doing calf stretches for 30 to 45 seconds several times per day. Protect the heel. The shoe may need to be modified to provide the proper heel lift or arch support. Select a shoe with good arch support and heel lift if possible. Try heel lifts or heel cups in sports shoes, especially cleats. Try arch support in cleats if flat feet contribute to the problem.
Aggressive Achilles Tendon Rupture Rehabilitation Program
Overview
 The Achilles tendon is the largest tendon in the body. It connects your calf muscles to your heel bone and is used when you walk, run, and jump. Although the Achilles tendon can withstand great stresses from running and jumping, it is vulnerable to injury. A rupture of the tendon is a tearing and separation of the tendon fibers so that the tendon can no longer perform its normal function.
The Achilles tendon is the largest tendon in the body. It connects your calf muscles to your heel bone and is used when you walk, run, and jump. Although the Achilles tendon can withstand great stresses from running and jumping, it is vulnerable to injury. A rupture of the tendon is a tearing and separation of the tendon fibers so that the tendon can no longer perform its normal function.
Causes
There are a number of factors that can increase the risk of an Achilles tendon rupture, which include the following. You?re most likely to rupture your Achilles tendon during sports that involve bursts of jumping, pivoting and running, such as football or tennis. Your Achilles tendon becomes less flexible and less able to absorb repeated stresses, for example of running, as you get older. Small tears can develop in the fibres of the tendon and it may eventually completely tear. There is a very small risk of an Achilles tendon rupture if you have Achilles tendinopathy (also called Achilles tendinitis). This is where your tendon breaks down, which causes pain and stiffness in your Achilles tendon, both when you exercise and afterwards. If you take quinolone antibiotics and corticosteroid medicines, it can increase your risk of an Achilles tendon injury, particularly if you take them together. The exact reasons for this aren't fully understood at present.
Symptoms
Although it's possible to have no signs or symptoms with an Achilles tendon rupture, most people experience pain, possibly severe, and swelling near your heel. An inability to bend your foot downward or "push off" the injured leg when you walk. An inability to stand up on your toes on the injured leg. A popping or snapping sound when the injury occurs. Seek medical advice immediately if you feel a pop or snap in your heel, especially if you can't walk properly afterward.
Diagnosis
Other less serious causes of pain in the back of the lower leg include Achilles tendonitis or bursitis. To distinguish between these possibilities, your physician will take a thorough history and examine your lower leg to look for signs of a rupture. The presence of a defect in the tendon that can be felt, evidence of weakness with plantarflexion, and a history consistent with Achilles tendon rupture are usually sufficient for diagnosis. Your physician may also perform a ?Thompson test,? which consists of squeezing the calf muscles of the affected leg. With an intact Achilles tendon, the foot will bend downward; however, with a complete rupture of the tendon, the foot will not move. In cases where the diagnosis is equivocal, your physician may order an MRI of the leg to diagnose a rupture of the Achilles tendon.
Non Surgical Treatment
A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. Use support devices as directed. You may need crutches or a cane for support when you walk. These devices help decrease stress and pressure on your tendon. Your caregiver will tell you how much weight you can put on your leg. Ask for more information about how to use crutches or a cane correctly. Start activity as directed. Your caregiver will tell you when it is okay to walk and play sports. You may not be able to play sports for 6 months or longer. Ask when you can go back to work or school. Do not drive until your caregiver says it is okay. 
Surgical Treatment
Surgery to repair an Achilles tendon rupture is performed under a spinal or general anaesthetic. During surgery the surgeon makes an incision in the skin over the ruptured portion of the tendon. The tendon ends are located and joined together with strong sutures (stitches), allowing the tendon to closely approximate its previous length. The skin is then closed with sutures and the foot is immobilised in a cast or splint, again in the toes-pointed position. Seven to ten days after surgery the cast or splint is removed in order for the sutures in the skin to be removed. Another cast or splint will be applied and will stay in place a further 5 - 7 weeks.
Prevention
To help prevent an Achilles tendon injury, it is a good practice to perform stretching and warm-up exercises before any participating in any activities. Gradually increase the intensity and length of time of activity. Muscle conditioning may help to strengthen the muscles in the body.
Leg Length Discrepancy Following Hip Replacement Surgery
While many people have slight differences in the length of one leg compared to the other, a significant difference between the two legs can cause problems. Leg length discrepancies can disturb the way a person walks, how his or her spine lines up and strain hip joints.

Causes
Leg discrepancy can develop from a medical issue in any portion of the femur or tibia. One leg may lengthen, but leg shortening is much more common. Factors that can cause leg length discrepancy include inherited growth deficiencies. Infections. A bone infection can cause delayed growth in the affected limb. Injury. If your child breaks a leg, it may be shorter once it heals. This is most likely to happen if the fracture or break was complicated, an open fracture, or an injury that affected the growth plate near the end of the bone. Alternatively, a break can cause bones to grow faster after healing, making a leg longer. Tumors. Legg-Calve-Perthes disease. This is a condition that affects the ball (femoral head) of the hip joint. The femoral head may be friable and damage easily, sometimes leading to shortening of the thigh bone. Hemihypertrophy. In children with this condition, one side of the body grows more quickly than the other. Vascular malformations. These are abnormal clusters of veins and arteries that can form close to the bone and stimulate growth. Juvenile arthritis. Inflammation from arthritis can stimulate growth in the affected leg and cause discrepancy.
Symptoms
The effects vary from patient to patient, depending on the cause of the discrepancy and the magnitude of the difference. Differences of 3 1/2 to 4 percent of the total length of the lower extremity (4 cm or 1 2/3 inches in an average adult), including the thigh, lower leg and foot, may cause noticeable abnormalities while walking and require more effort to walk. Differences between the lengths of the upper extremities cause few problems unless the difference is so great that it becomes difficult to hold objects or perform chores with both hands. You and your physician can decide what is right for you after discussing the causes, treatment options and risks and benefits of limb lengthening, including no treatment at all. Although an LLD may be detected on a screening examination for curvature of the spine (scoliosis), LLD does not cause scoliosis. There is controversy about the effect of LLD on the spine. Some studies indicate that people with an LLD have a greater incidence of low back pain and an increased susceptibility to injuries, but other studies refute this relationship.
Diagnosis
There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference.
Non Surgical Treatment
You may be prescribed a heel lift, which will equal out your leg length and decrease stress on your low back and legs. If it?s your pelvis causing the leg length discrepancy, then your physical therapist could use your muscles to realign your pelvis and then strengthen your core/abdominal region to minimize the risk of such malalignment happening again. If you think that one leg may be longer than the other and it is causing you to have pain or you are just curious, then make an appointment with a physical therapist.

Surgical Treatment
Surgical treatments vary in complexity. Sometimes the goal of surgery is to stop the growth of the longer limb. Other times, surgeons work to lengthen the shorter limb. Orthopedic surgeons may treat children who have limb-length conditions with one or a combination of these surgical techniques. Bone resection. An operation to remove a section of bone, evening out the limbs in teens or adults who are no longer growing. Epiphyseal stapling. An operation to slow the rate of growth of the longer limb by inserting staples into the growth plate, then removing them when the desired result is achieved. Epiphysiodesis. An operation to slow the rate of growth of the longer limb by creating a permanent bony ridge near the growth plate. Limb lengthening. A procedure (also called distraction osteogenesis or the Ilizarov procedure) that involves attaching an internal or external fixator to a limb and gradually pulling apart bone segments to grow new bone between them. There are several ways your doctor can predict the final LLD, and thus the timing of the surgery. The easiest way is the so-called Australian method, popularised by Dr. Malcolm Menelaus, an Australian orthopedic surgeon. According to this method, growth in girls is estimated to stop at age 14, and in boys at age 16 years. The femur grows at the rate of 10 mm. a year, and the upper tibia at the rate of 6 mm. a year. Using simple arithmetic, one can get a fairly good prediction of future growth. This of course, is an average, and the patient may be an average. To cut down the risk of this, the doctor usually measures leg length using special X-ray technique (called a Scanogram) on three occasions over at least one year duration to estimate growth per year. He may also do an X-ray of the left hand to estimate the bone age (which in some cases may differ from chronological age) by comparing it with an atlas of bone age. In most cases, however, the bone age and chronological age are quite close. Another method of predicting final LLD is by using Anderson and Green?s remaining growth charts. This is a very cumbersome method, but was till the 1970?s, the only method of predicting remaining growth. More recently, however, a much more convenient method of predicting LLD was discovered by Dr. Colin Moseley from Montreal. His technique of using straight line graphs to plot growth of leg lengths is now the most widely used method of predicting leg length discrepancy. Whatever method your doctor uses, over a period of one or two years, once he has a good idea of the final LLD, he can then formulate a plan to equalize leg lengths. Epiphyseodesis is usually done in the last 2 to 3 years of growth, giving a maximum correction of about 5 cm. Leg lengthening can be done at any age, and can give corrections of 5 to10 cm., or more.
Does Adult Aquired FlatFeet Require Surgical Teatments ?
Overview
Most flat feet are not painful, particularly those flat feet seen in children. In the adult acquired flatfoot, pain occurs because soft tissues (tendons and ligaments) have been torn. The deformity progresses or worsens because once the vital ligaments and posterior tibial tendon are lost, nothing can take their place to hold up the arch of the foot. The painful, progressive adult acquired flatfoot affects women four times as frequently as men. It occurs in middle to older age people with a mean age of 60 years. Most people who develop the condition already have flat feet. A change occurs in one foot where the arch begins to flatten more than before, with pain and swelling developing on the inside of the ankle. Why this event occurs in some people (female more than male) and only in one foot remains poorly understood. Contributing factors increasing the risk of adult acquired flatfoot are diabetes, hypertension, and obesity. 
Causes
There are numerous causes of acquired Adult Flatfoot, including, trauma, fracture, dislocation, tendon rupture/partial rupture or inflammation of the tendons, tarsal coalition, arthritis, neuroarthropathy and neurologic weakness. The most common cause of acquired Adult Flatfoot is due to overuse of a tendon on the inside of the ankle called the posterior tibial tendon. This is classed as - posterior tibial tendon dysfunction. What are the causes of Adult Acquired flat foot? Trauma, Fracture or dislocation. Tendon rupture, partial tear or inflammation. Tarsal Coalition. Arthritis. Neuroarthropathy. Neurological weakness.
Symptoms
The types of symptoms that may indicate Adult-Acquired Flat Foot Deformity include foot pain that worsens over time, loss of the arch, abnormal shoe wear (excessive wearing on the inner side of shoe from walking on the inner side of the foot) and an awkward appearance of the foot and ankle (when viewed from behind, heel and toes appear to go out to the side). It is important that we help individuals recognize the early symptoms of this condition, as there are many treatment options, depending upon the severity, the age of the patient, and the desired activity levels.
Diagnosis
The adult acquired flatfoot, secondary to posterior tibial tendon dysfunction, is diagnosed in a number of ways with no single test proven to be totally reliable. The most accurate diagnosis is made by a skilled clinician utilizing observation and hands on evaluation of the foot and ankle. Observation of the foot in a walking examination is most reliable. The affected foot appears more pronated and deformed compared to the unaffected foot. Muscle testing will show a strength deficit. An easy test to perform in the office is the single foot raise. A patient is asked to step with full body weight on the symptomatic foot, keeping the unaffected foot off the ground. The patient is then instructed to "raise up on the tip toes" of the affected foot. If the posterior tibial tendon has been attenuated or ruptured, the patient will be unable to lift the heel off the floor and rise onto the toes. In less severe cases, the patient will be able to rise on the toes, but the heel will not be noted to invert as it normally does when we rise onto the toes. X-rays can be helpful but are not diagnostic of the adult acquired flatfoot. Both feet - the symptomatic and asymptomatic - will demonstrate a flatfoot deformity on x-ray. Careful observation may show a greater severity of deformity on the affected side.
Non surgical Treatment
Because of the progressive nature of PTTD, early treatment is advised. If treated early enough, your symptoms may resolve without the need for surgery and progression of your condition can be arrested. In contrast, untreated PTTD could leave you with an extremely flat foot, painful arthritis in the foot and ankle, and increasing limitations on walking, running, or other activities. In many cases of PTTD, treatment can begin with non-surgical approaches that may include. Orthotic devices or bracing. To give your arch the support it needs, your foot and ankle surgeon may provide you with an ankle brace or a custom orthotic device that fits into the shoe. Immobilization. Sometimes a short-leg cast or boot is worn to immobilize the foot and allow the tendon to heal, or you may need to completely avoid all weight-bearing for a while. Physical therapy. Ultrasound therapy and exercises may help rehabilitate the tendon and muscle following immobilization. Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, help reduce the pain and inflammation. Shoe modifications. Your foot and ankle surgeon may advise changes to make with your shoes and may provide special inserts designed to improve arch support. 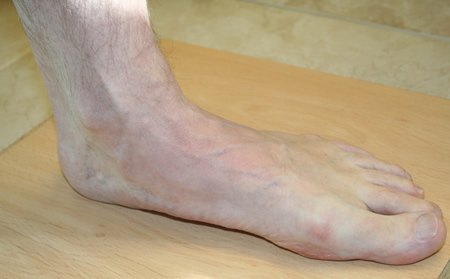
Surgical Treatment
Surgery should only be done if the pain does not get better after a few months of conservative treatment. The type of surgery depends on the stage of the PTTD disease. It it also dictated by where tendonitis is located and how much the tendon is damaged. Surgical reconstruction can be extremely complex. Some of the common surgeries include. Tenosynovectomy, removing the inflamed tendon sheath around the PTT. Tendon Transfer, to augment the function of the diseased posterior tibial tendon with a neighbouring tendon. Calcaneo-osteotomy, sometimes the heel bone needs to be corrected to get a better heel bone alignment. Fusion of the Joints, if osteoarthritis of the foot has set in, fusion of the joints may be necessary.